OUR PORTFOLIO
Real Medical Billing Work Across Leading Platforms
Explore our hands-on experience with major US insurance portals and billing systems, delivering accurate processing, reduced denials, and improved revenue outcomes.
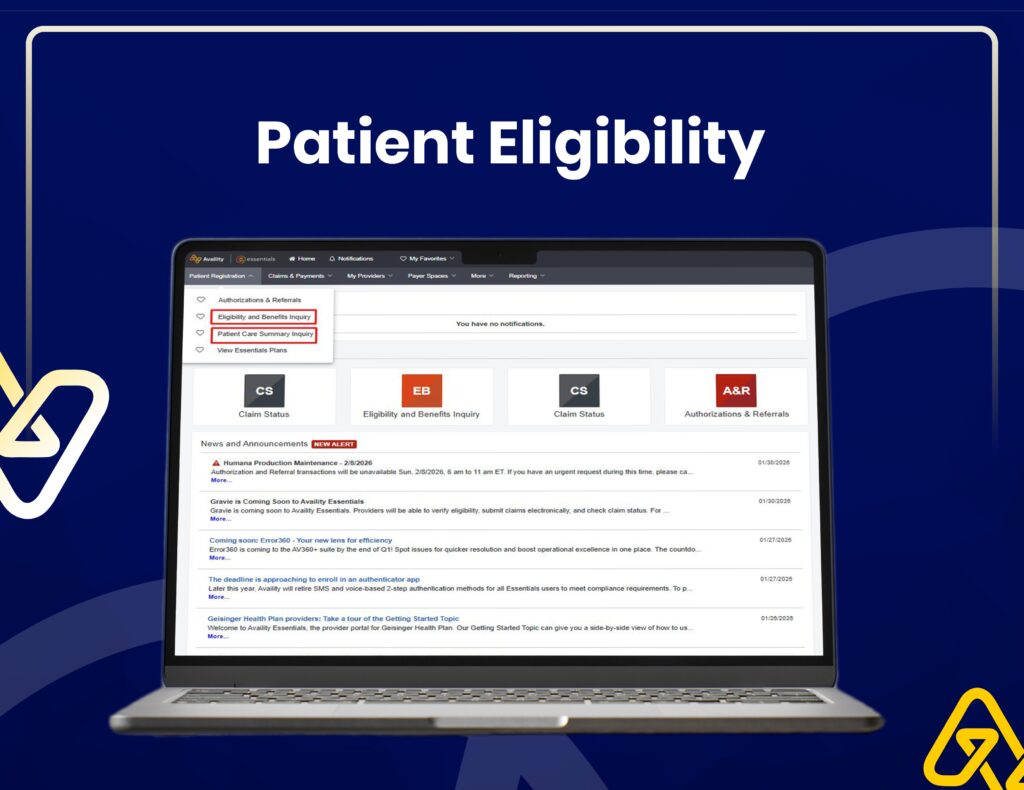
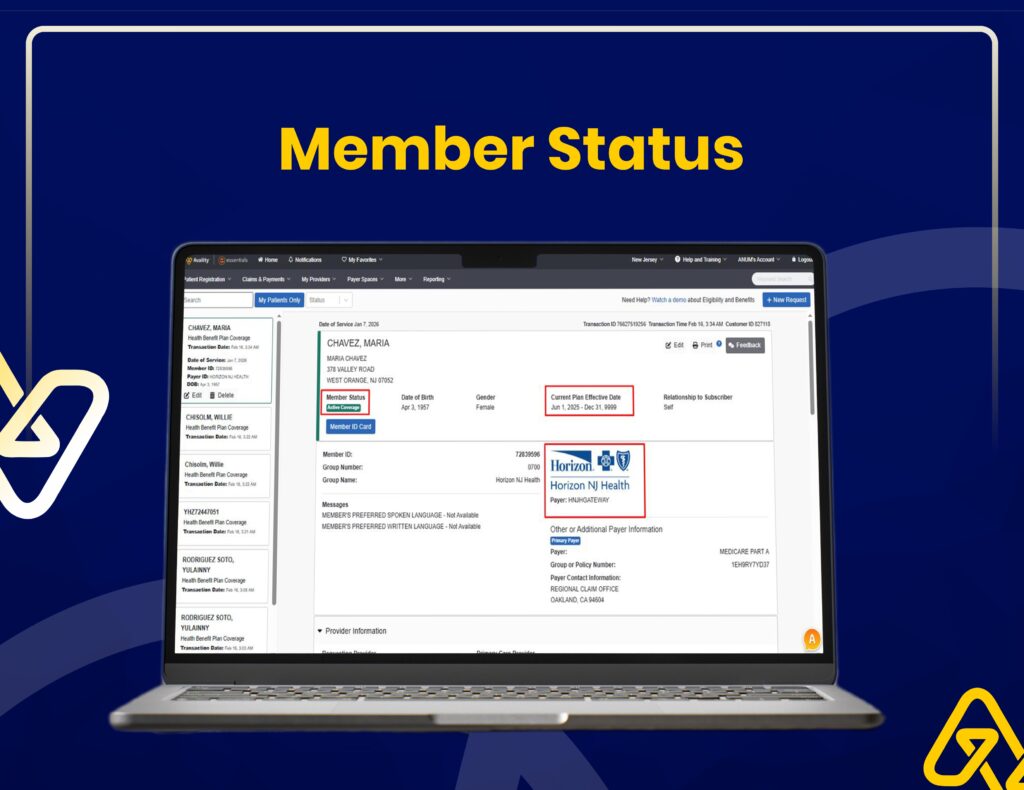
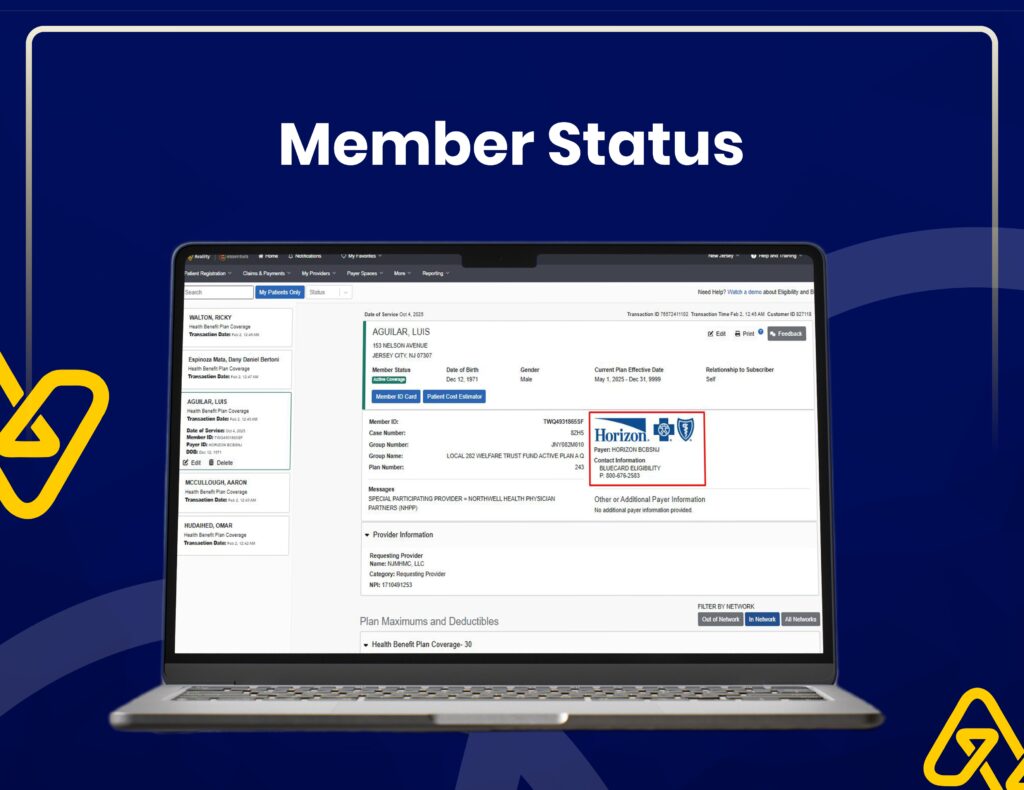
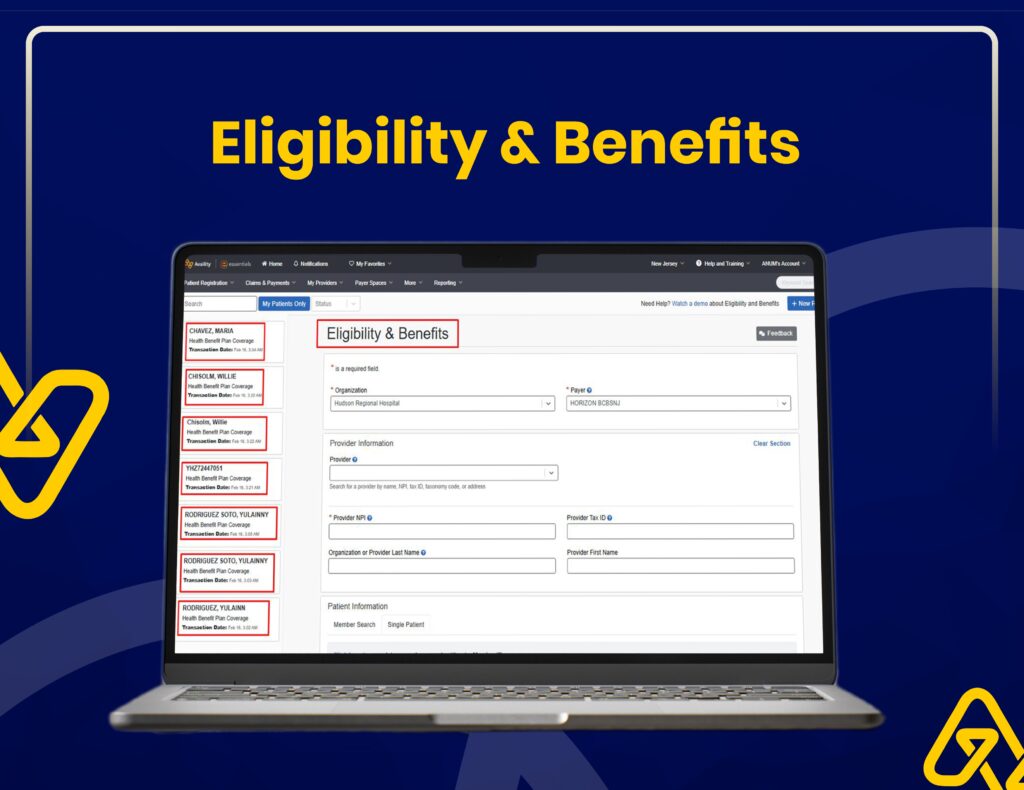
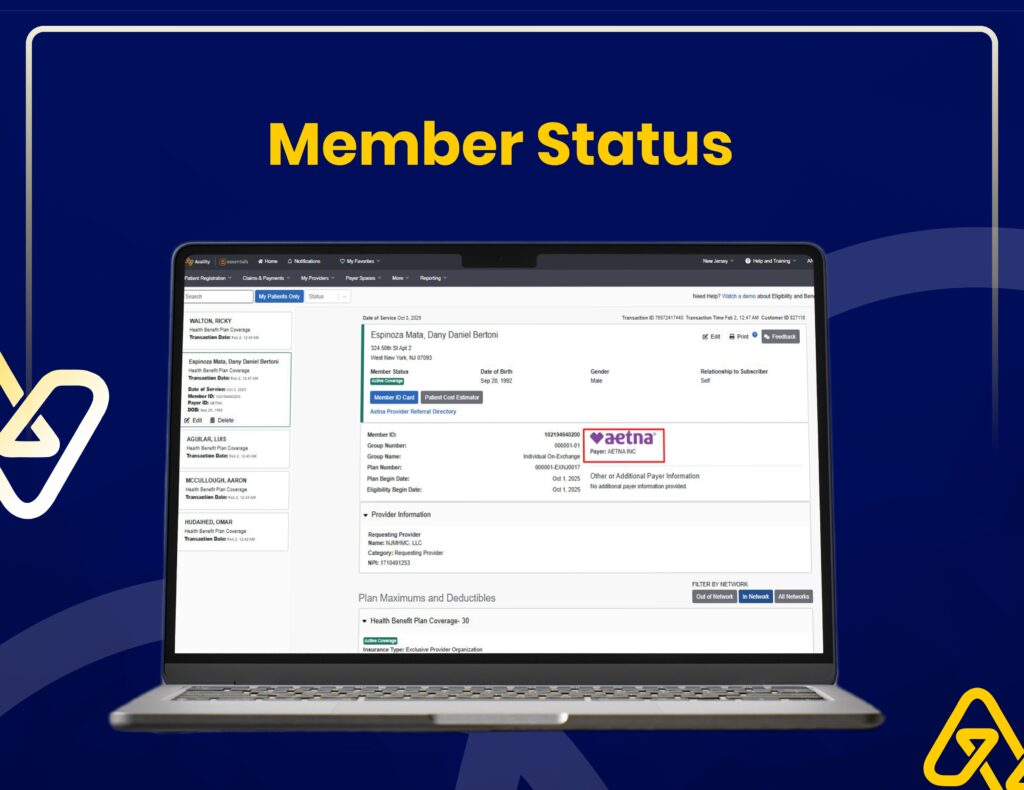
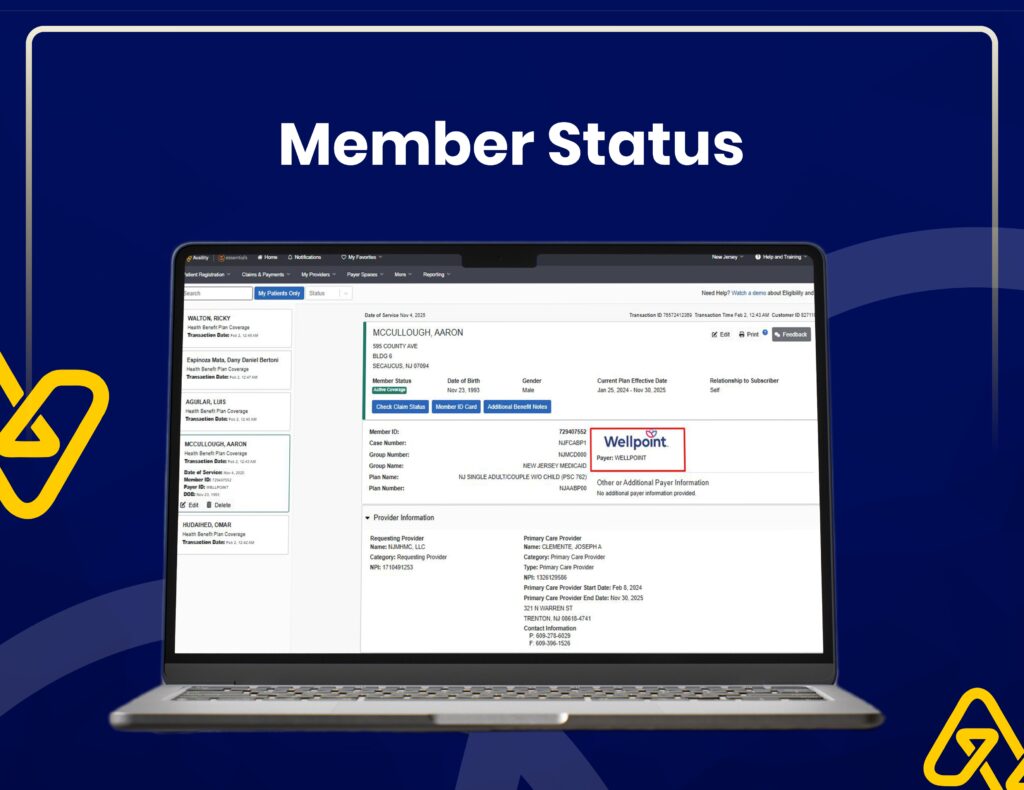
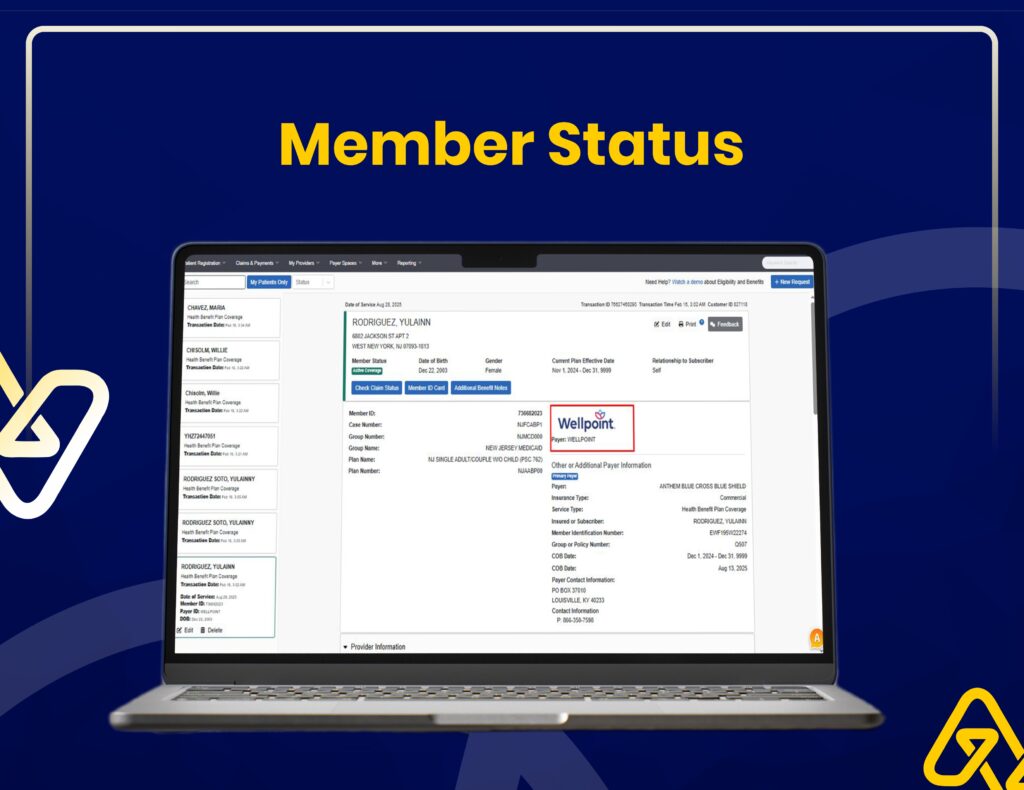
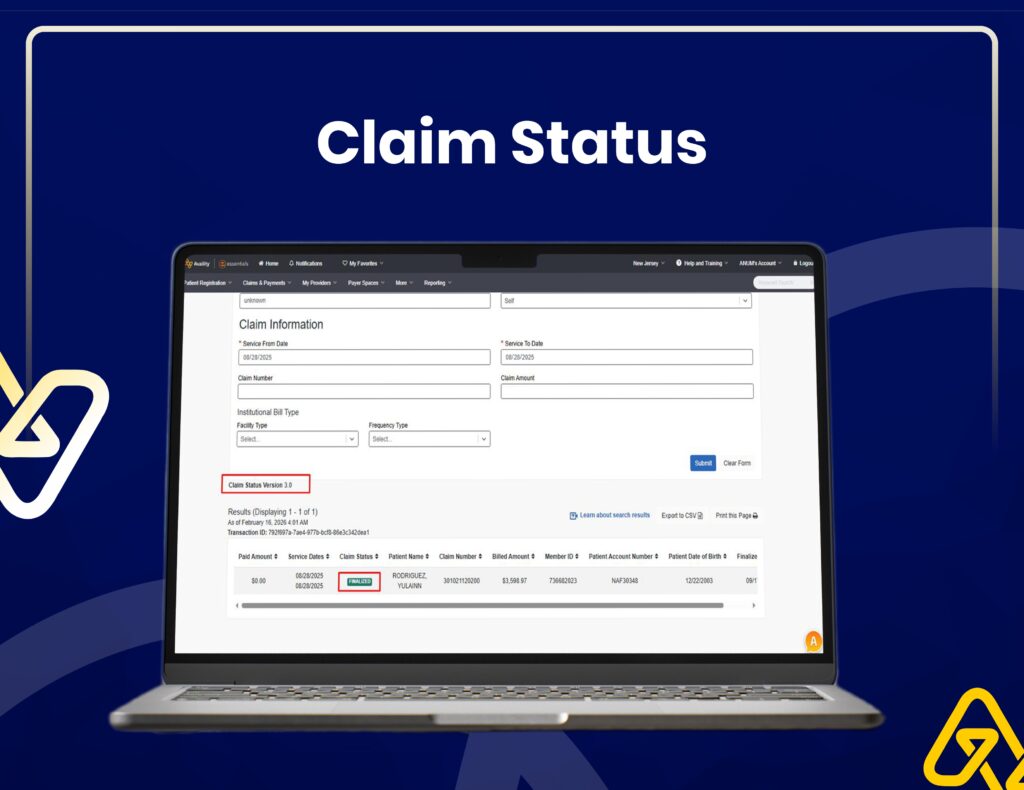
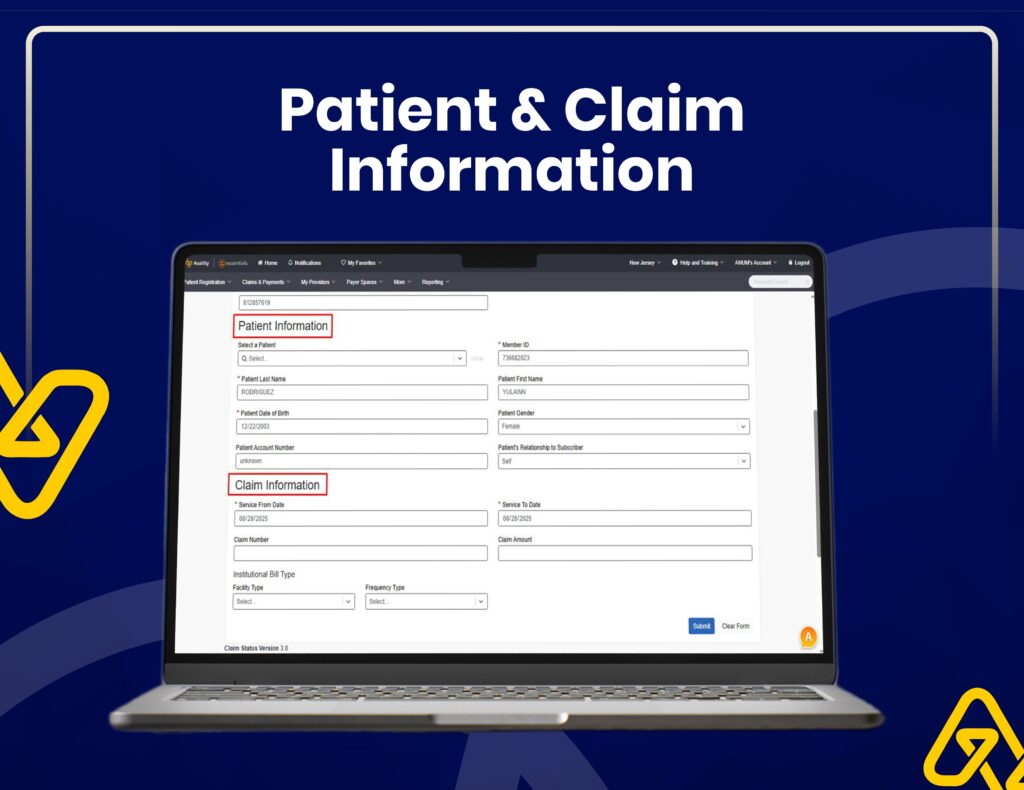
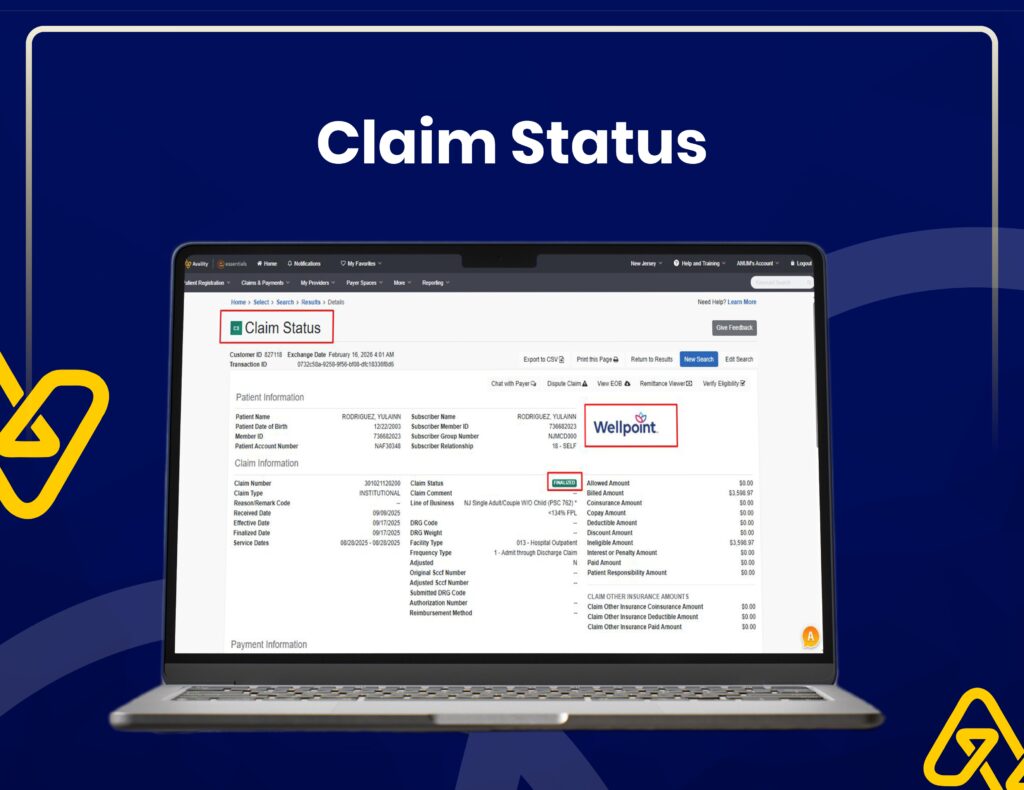
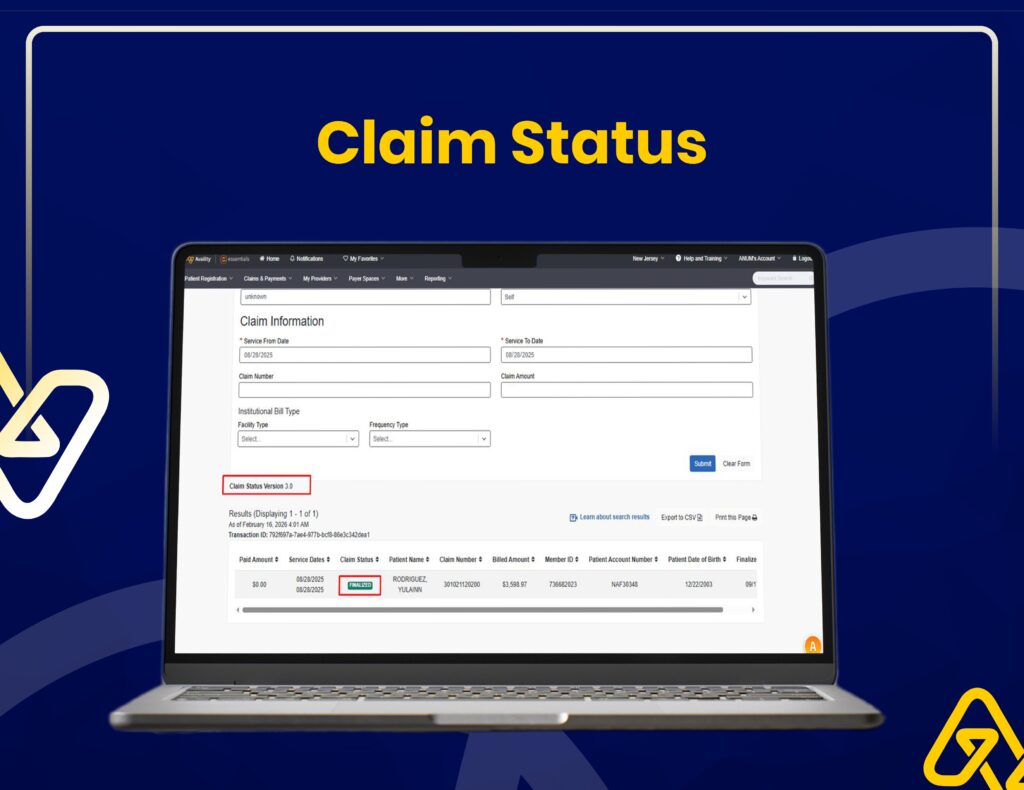
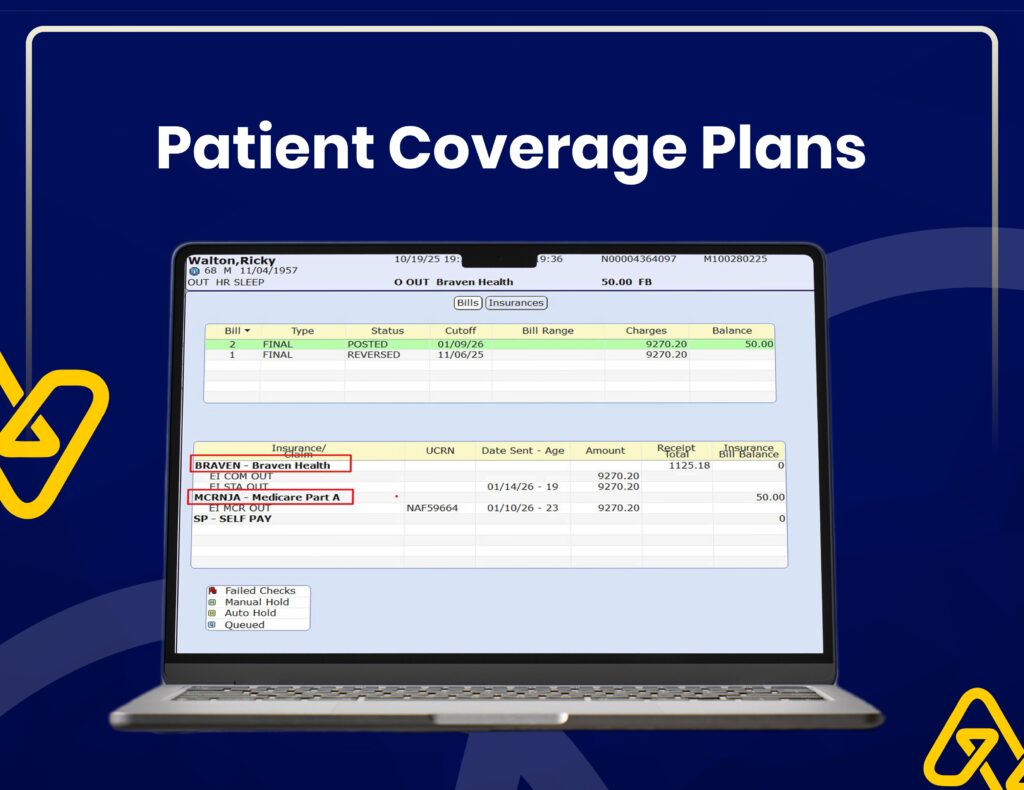
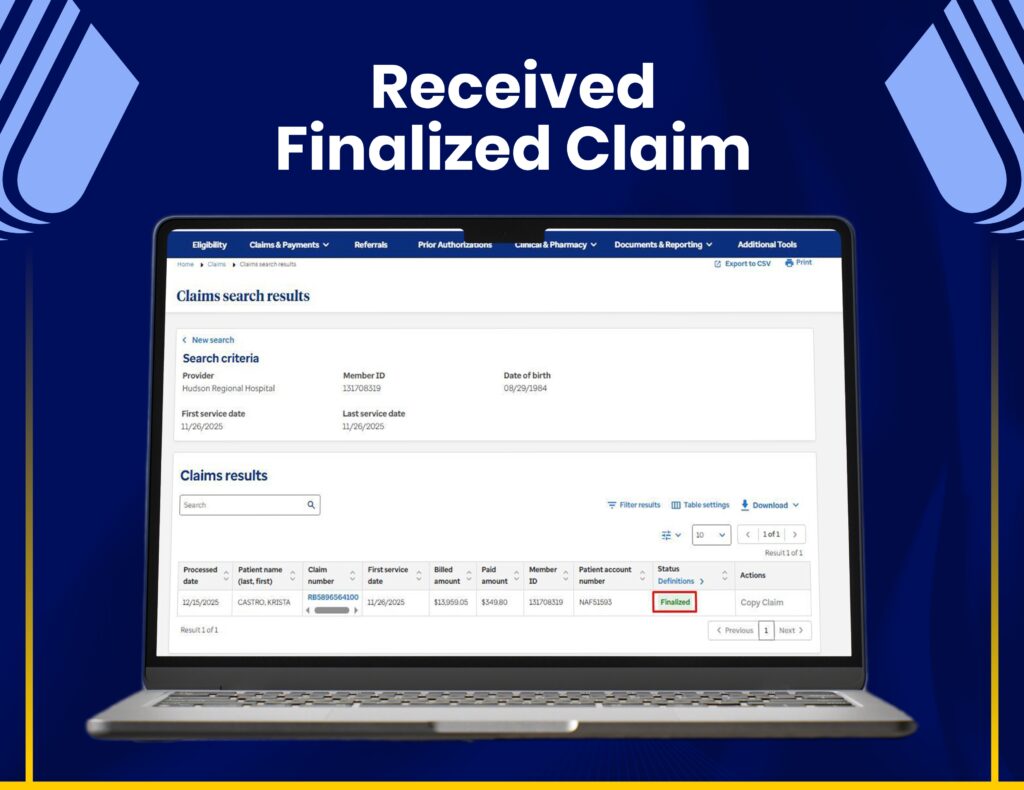
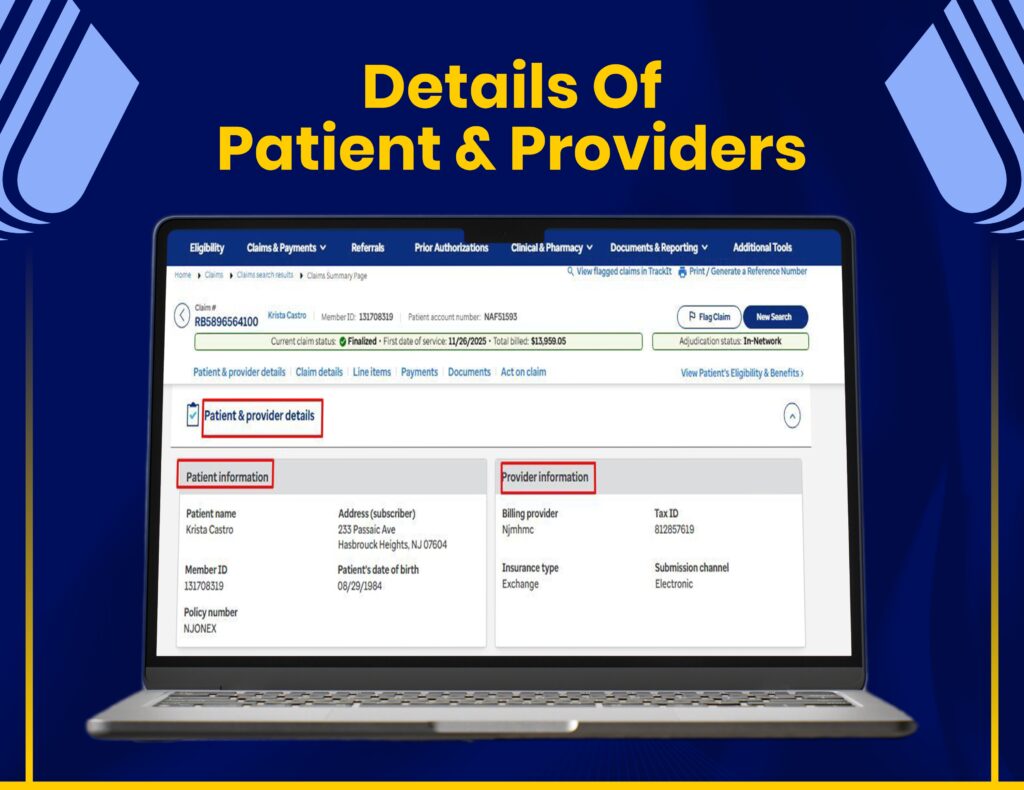
Insurance Verification & Claim Tracking
We use Availity for real-time eligibility checks, claim status tracking, and accurate insurance verification to reduce claim rejections.
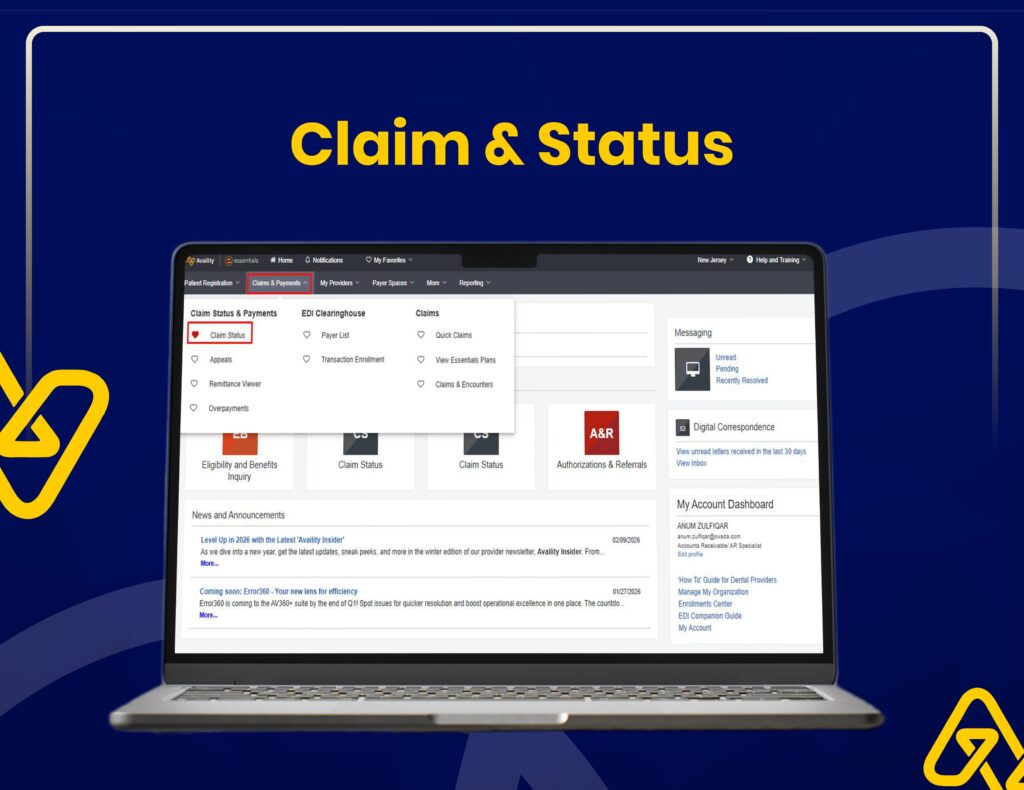
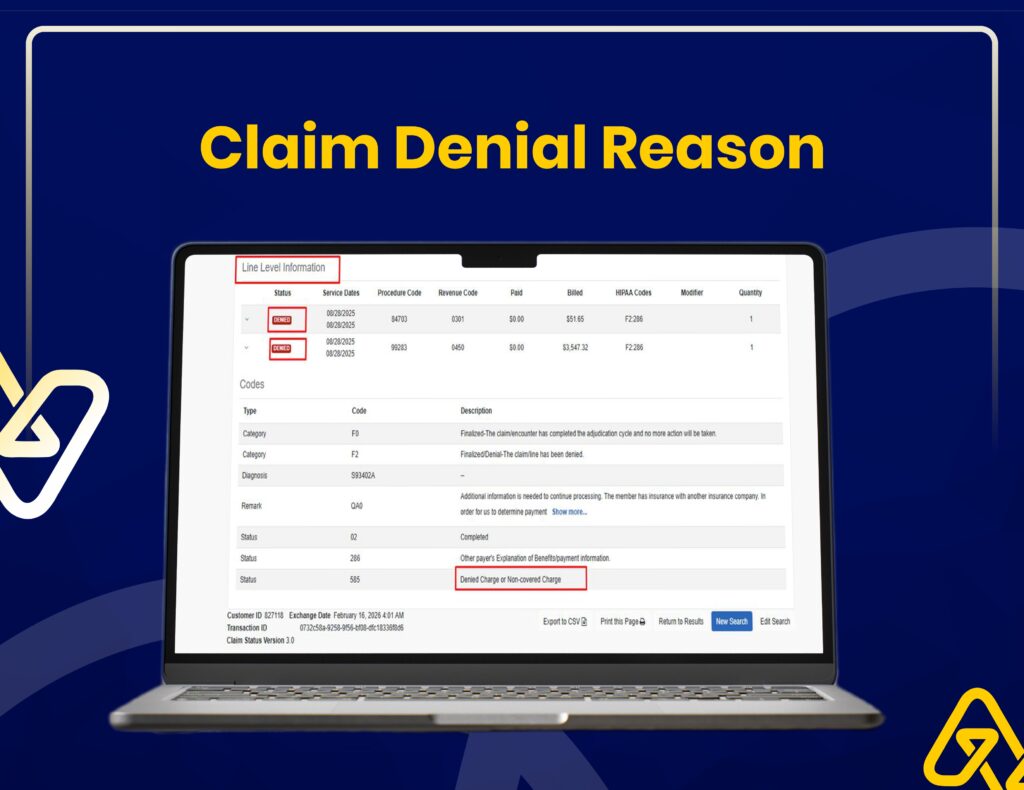
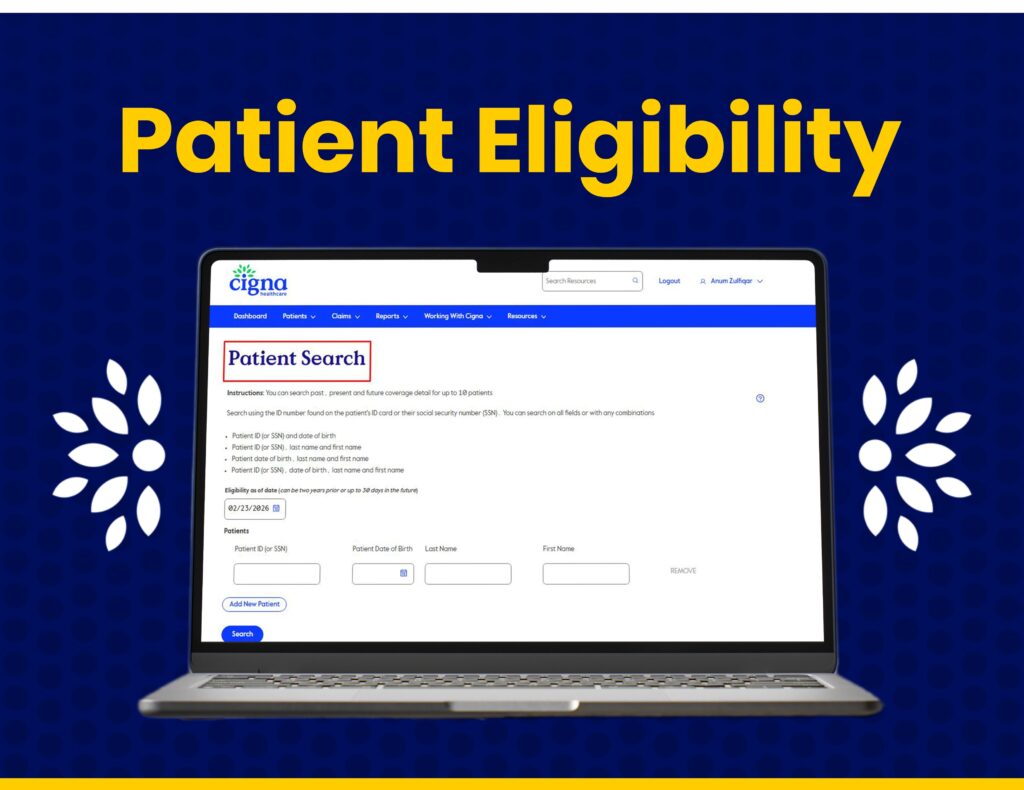
Claims Submission & Follow-Ups
Our team manages claim submissions, status monitoring, and denial follow-ups through the Cigna portal for faster approvals.
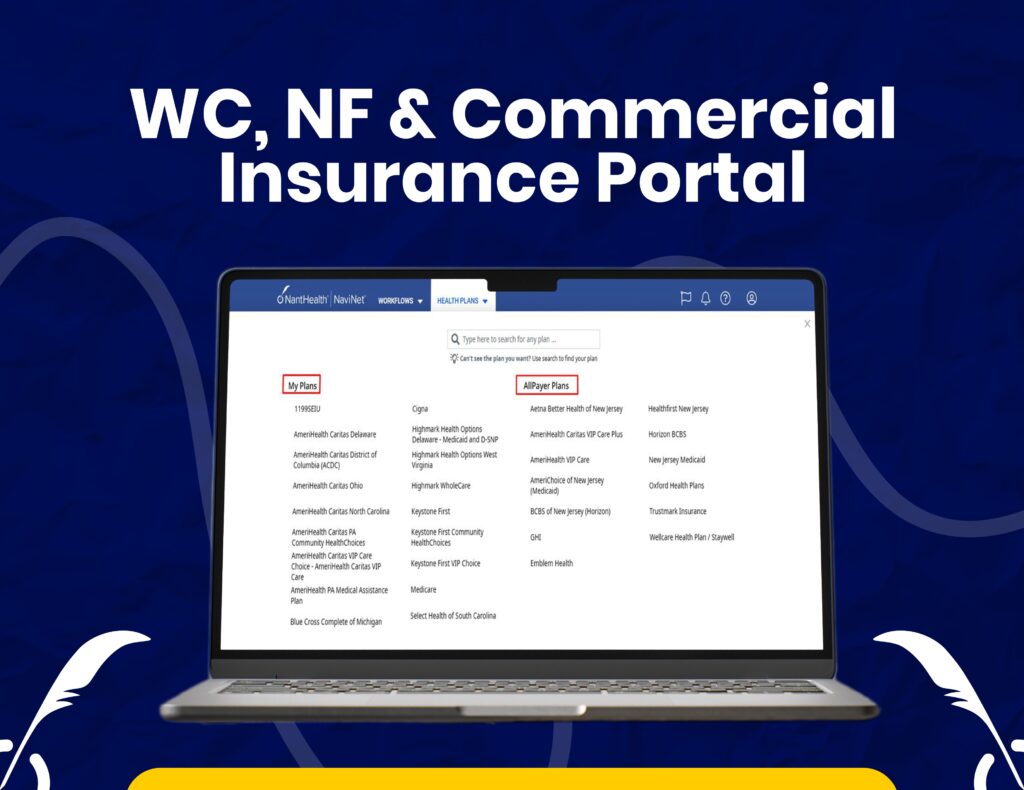
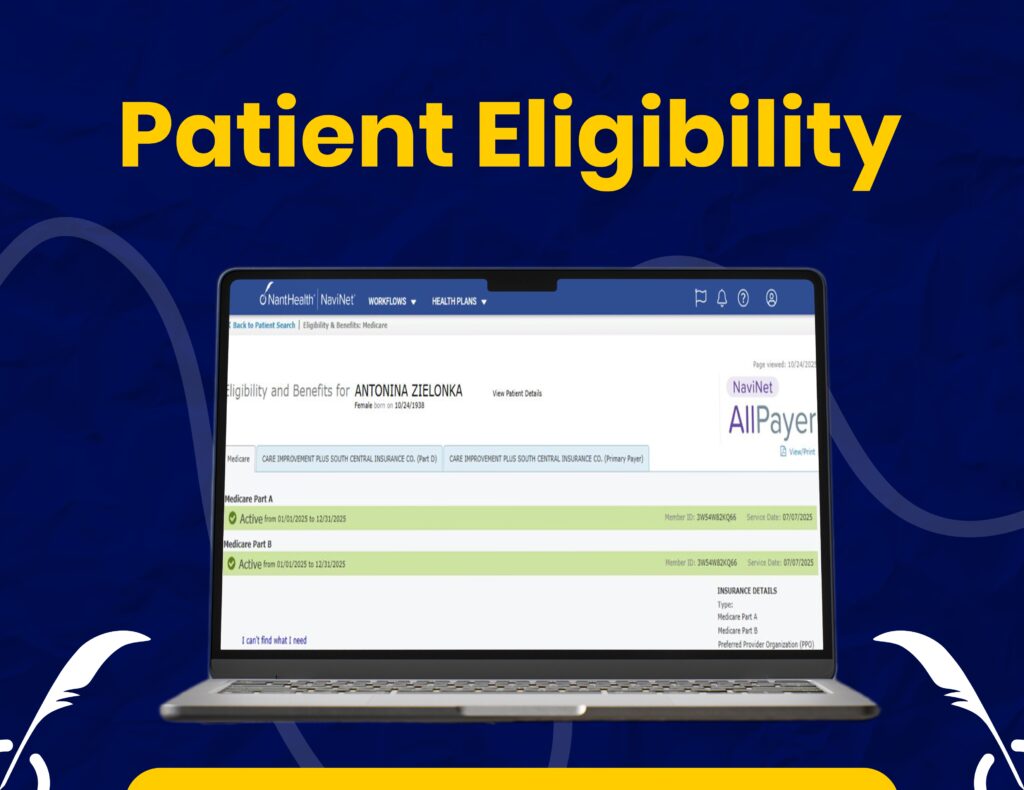
Real-Time Eligibility & Billing Workflow
We handle eligibility verification, claim processing, and payer communication using Navinet for efficient billing operations.
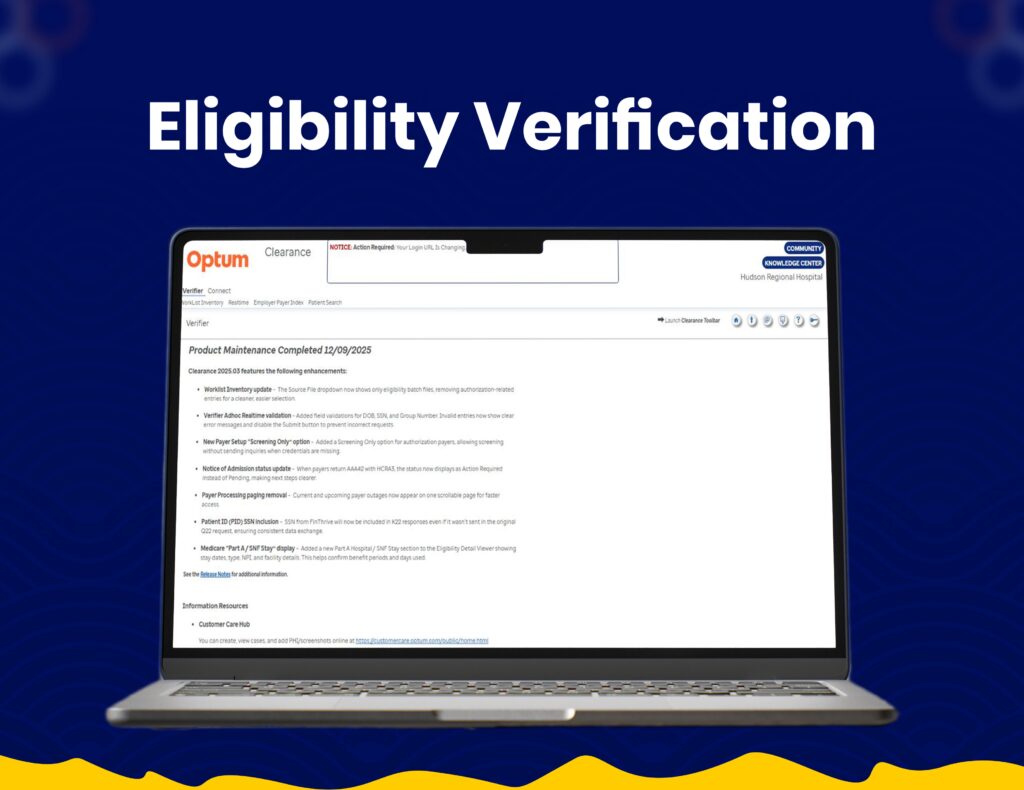
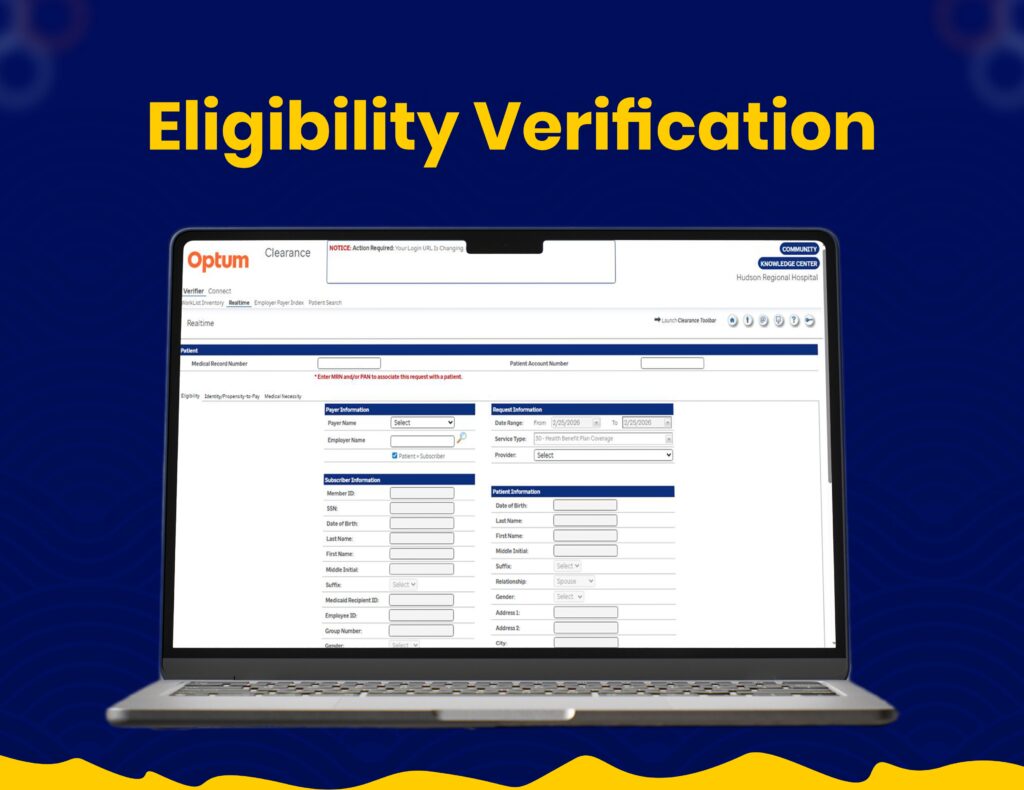
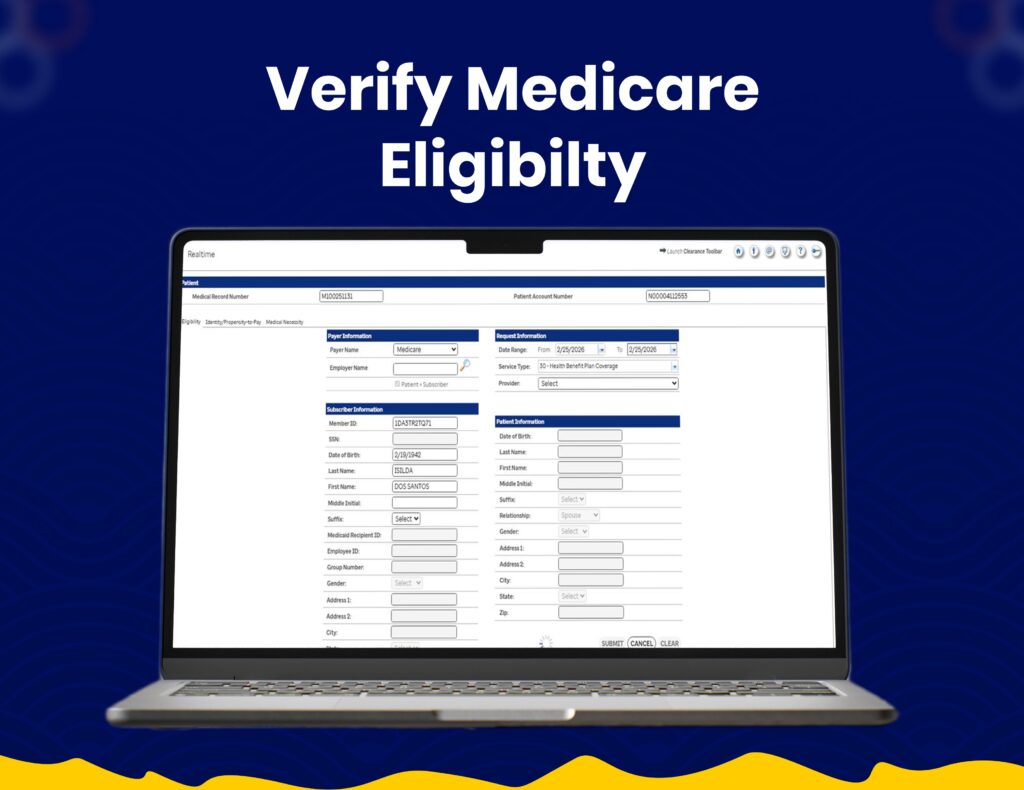
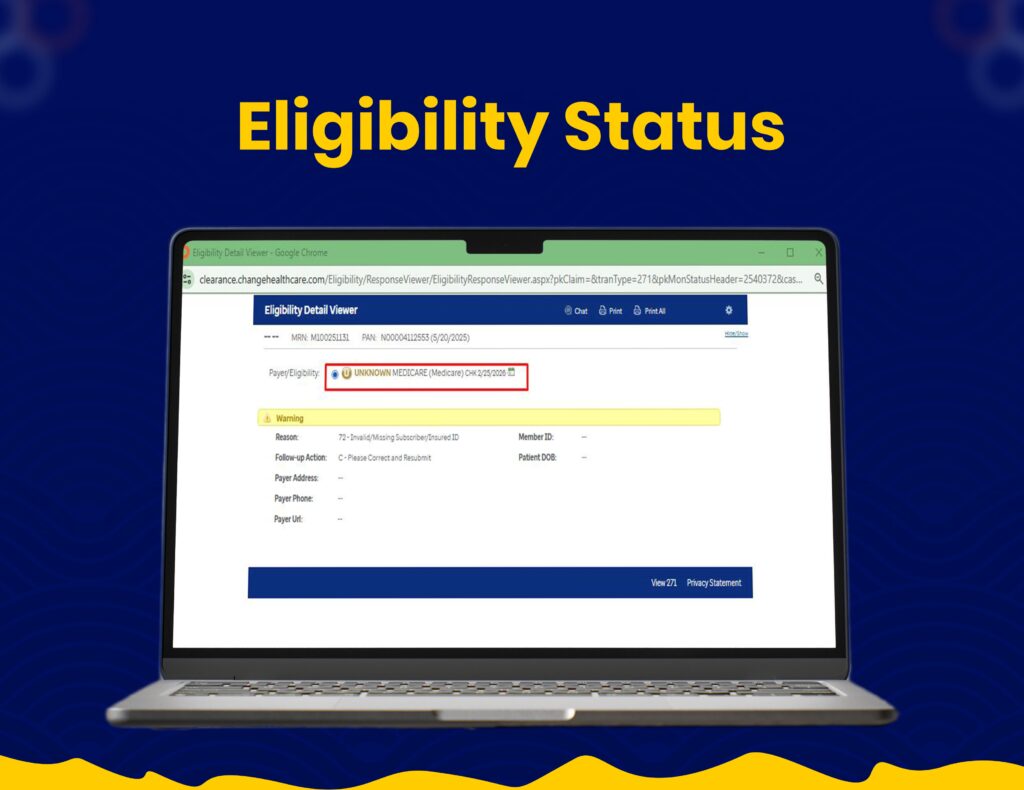
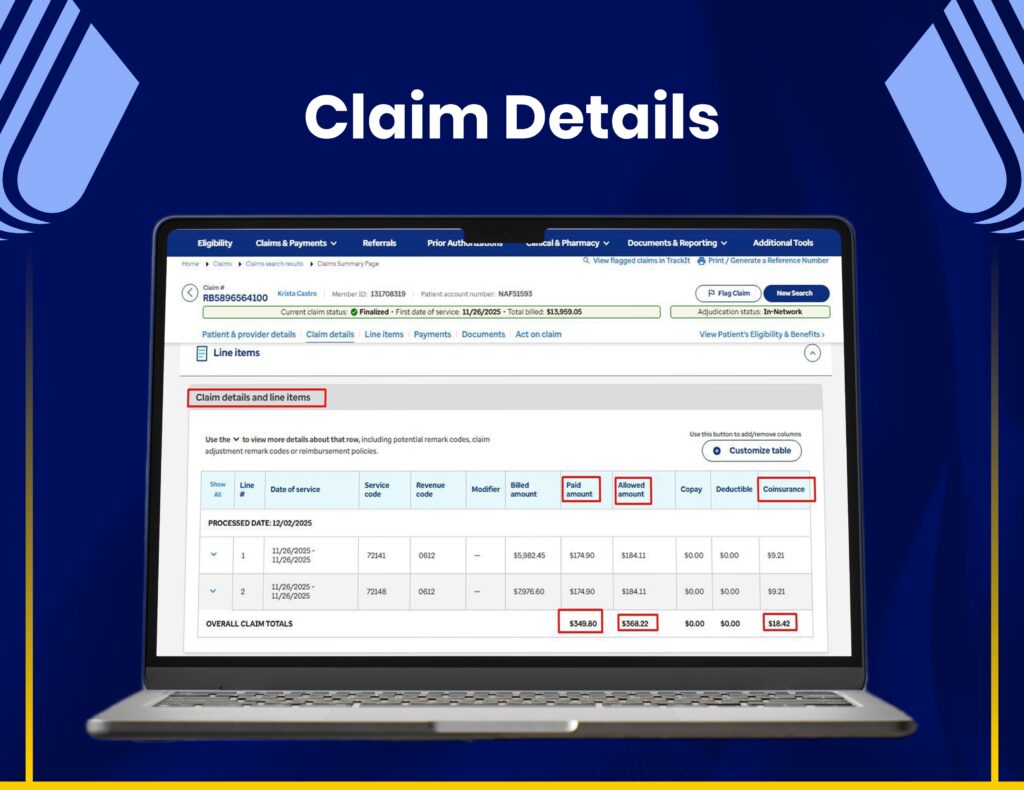
End-to-End Claim Processing
We utilize Optum systems for seamless claim submissions, tracking, and revenue cycle management with improved accuracy.
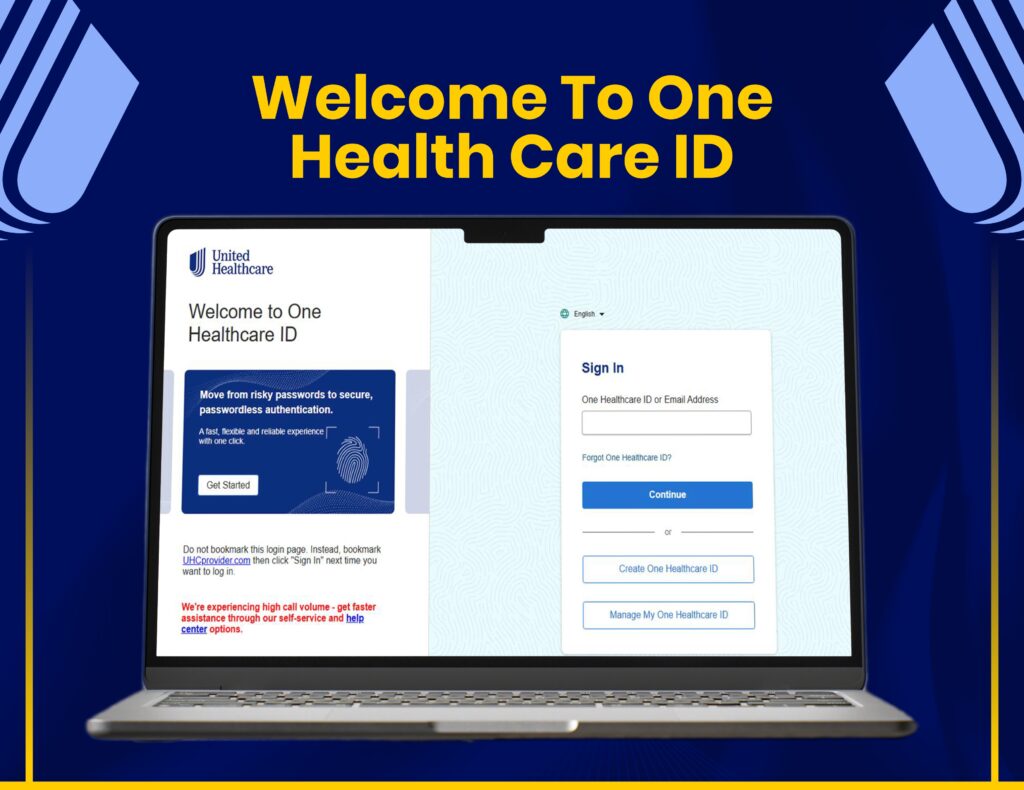
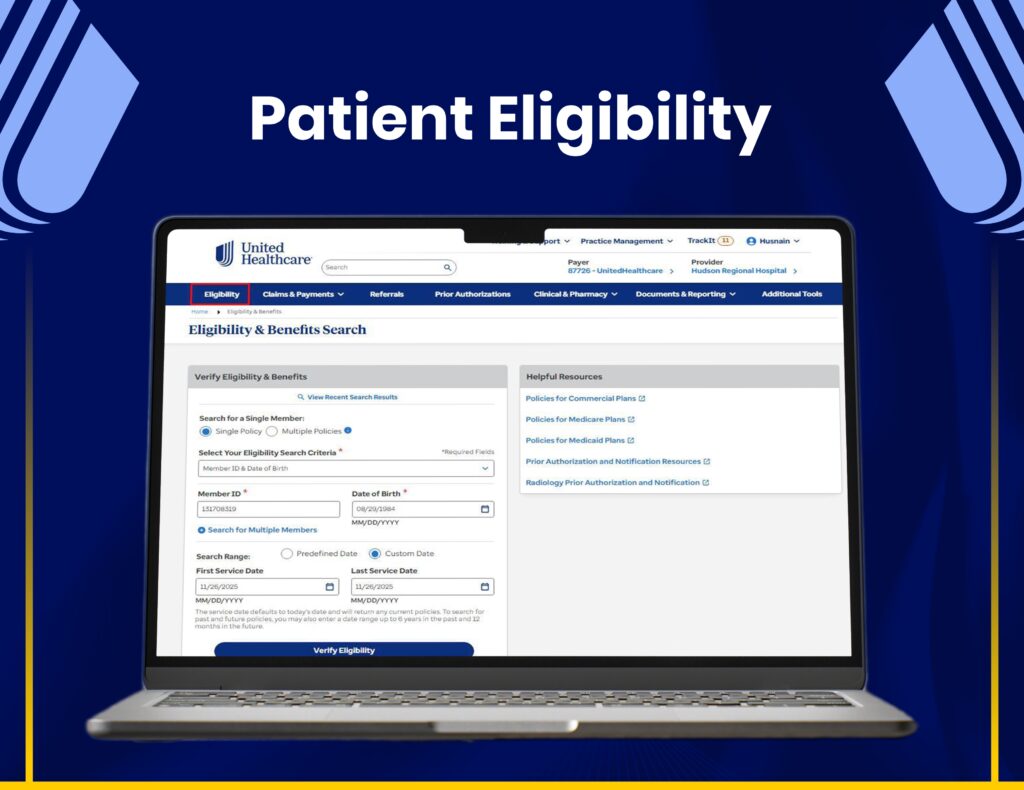
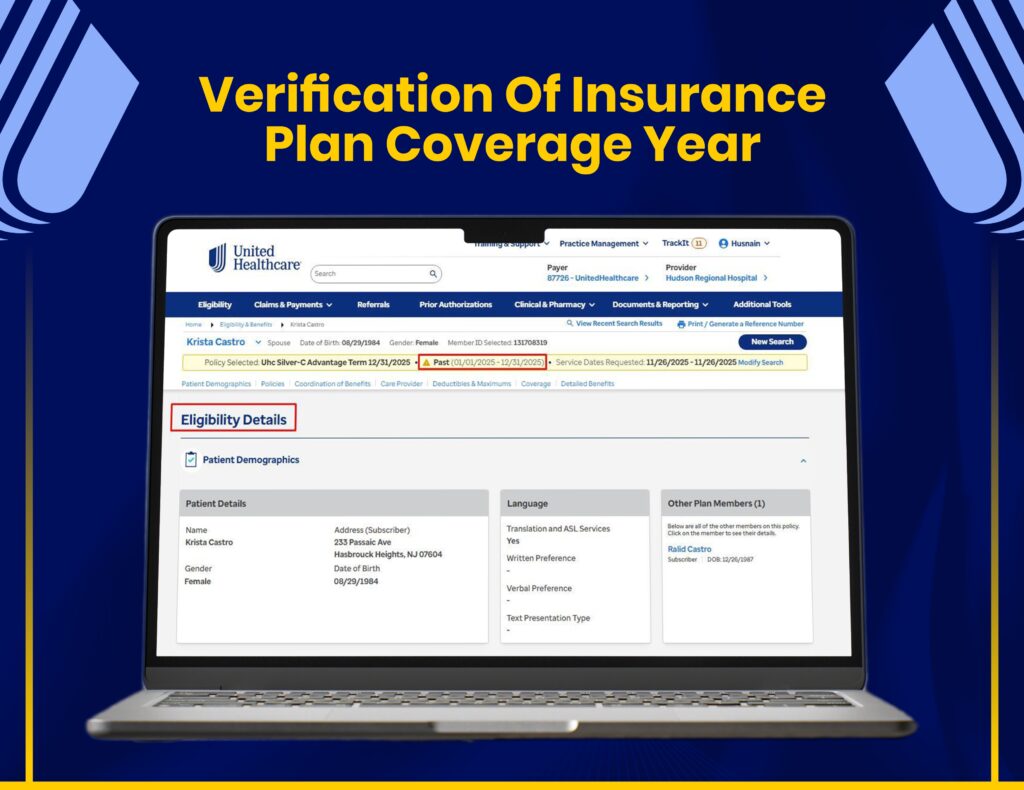
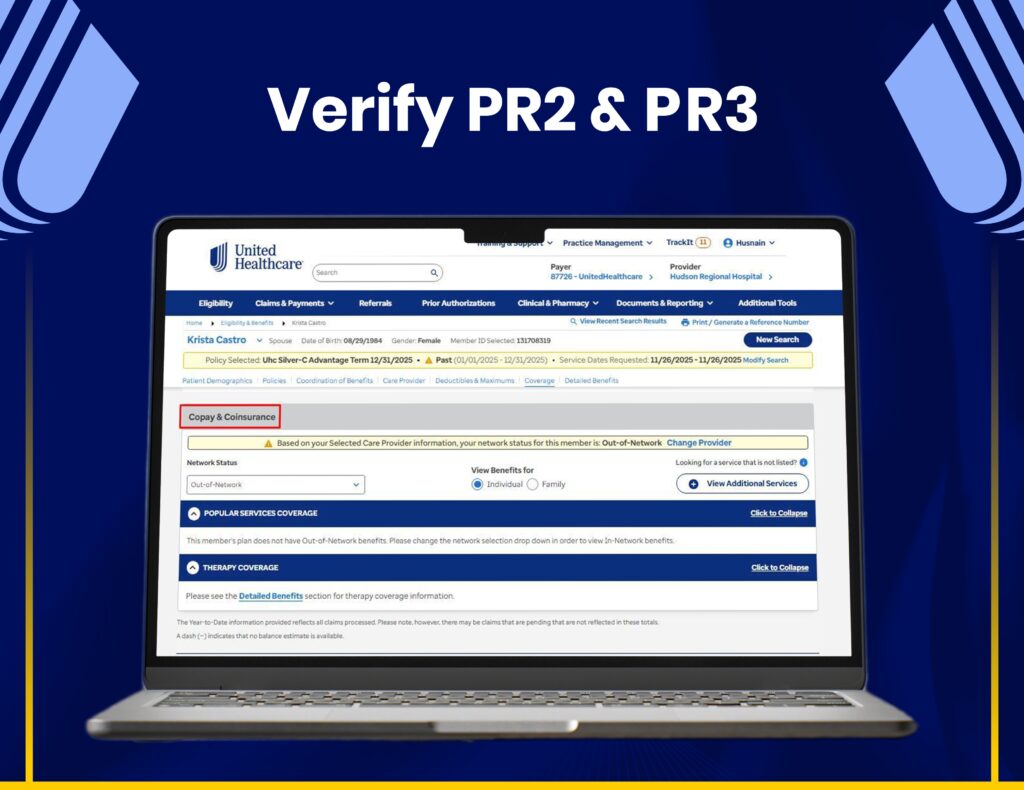
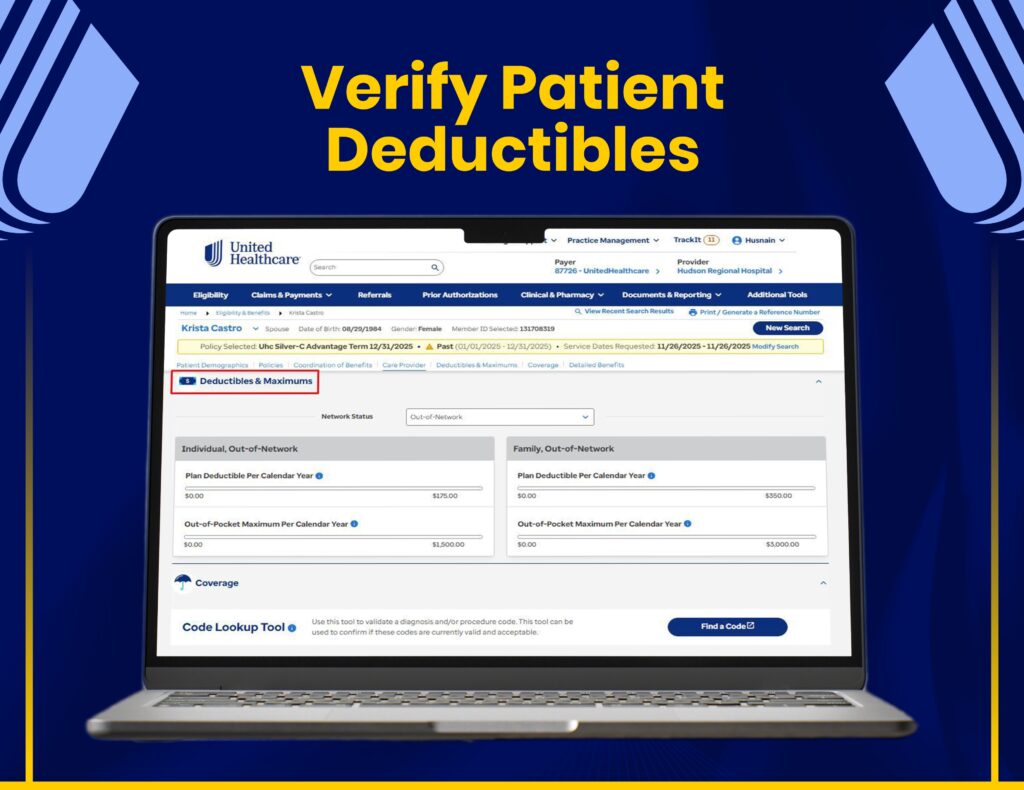
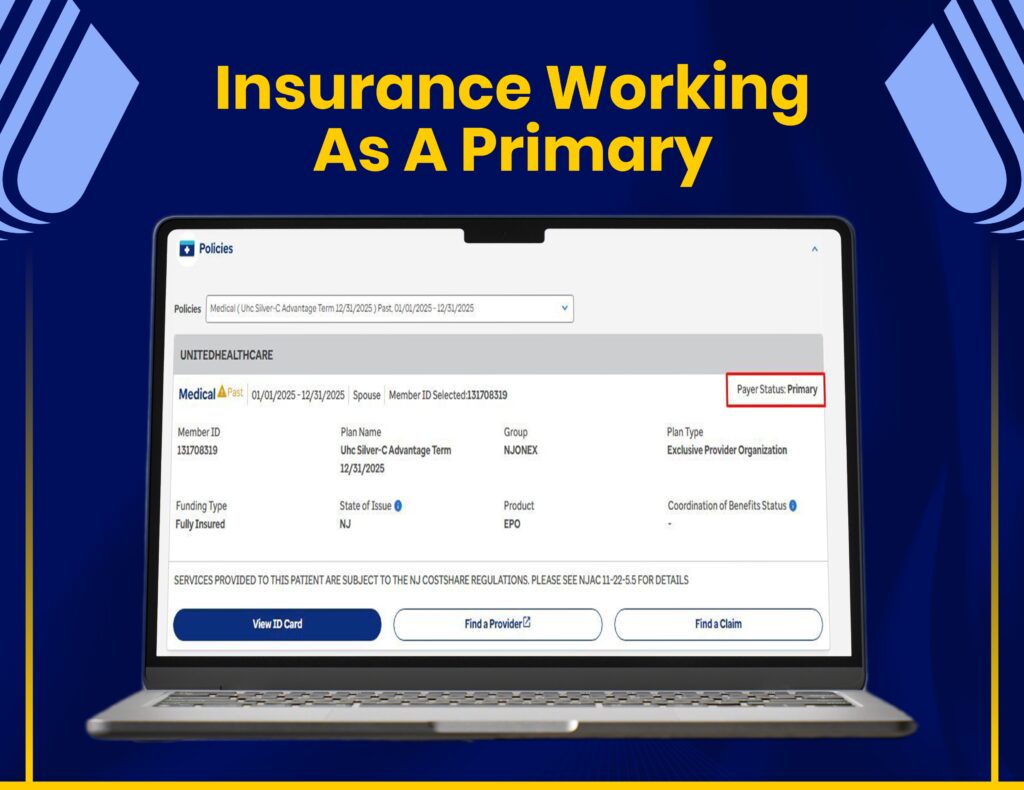
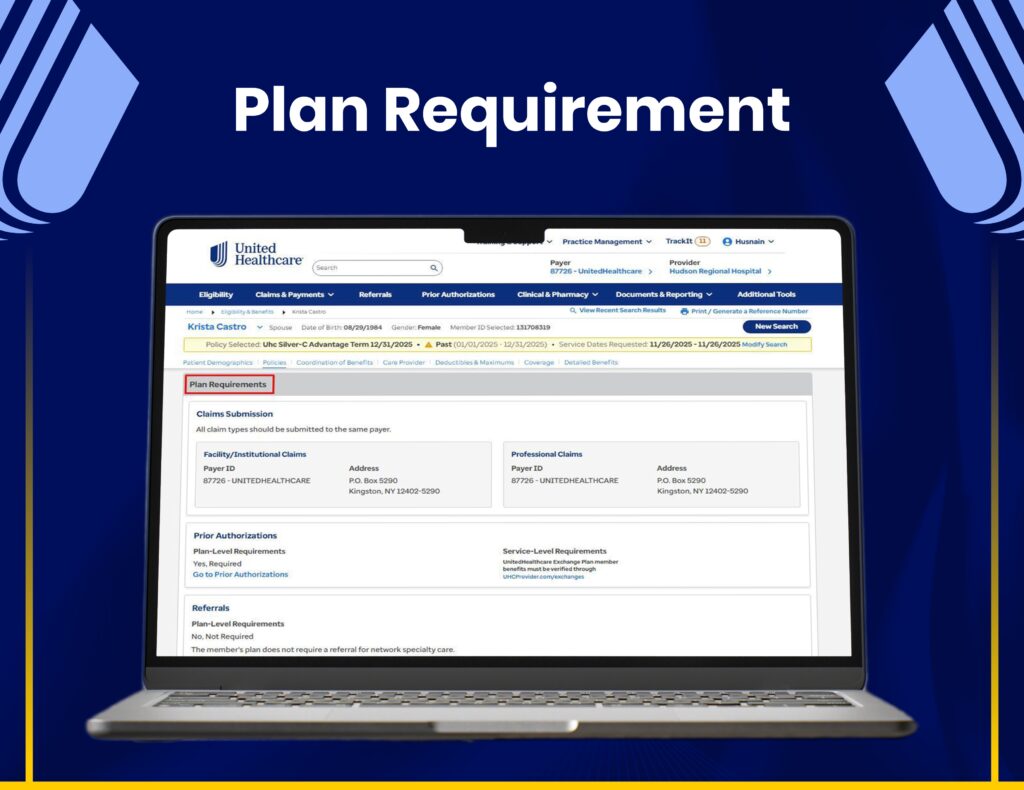
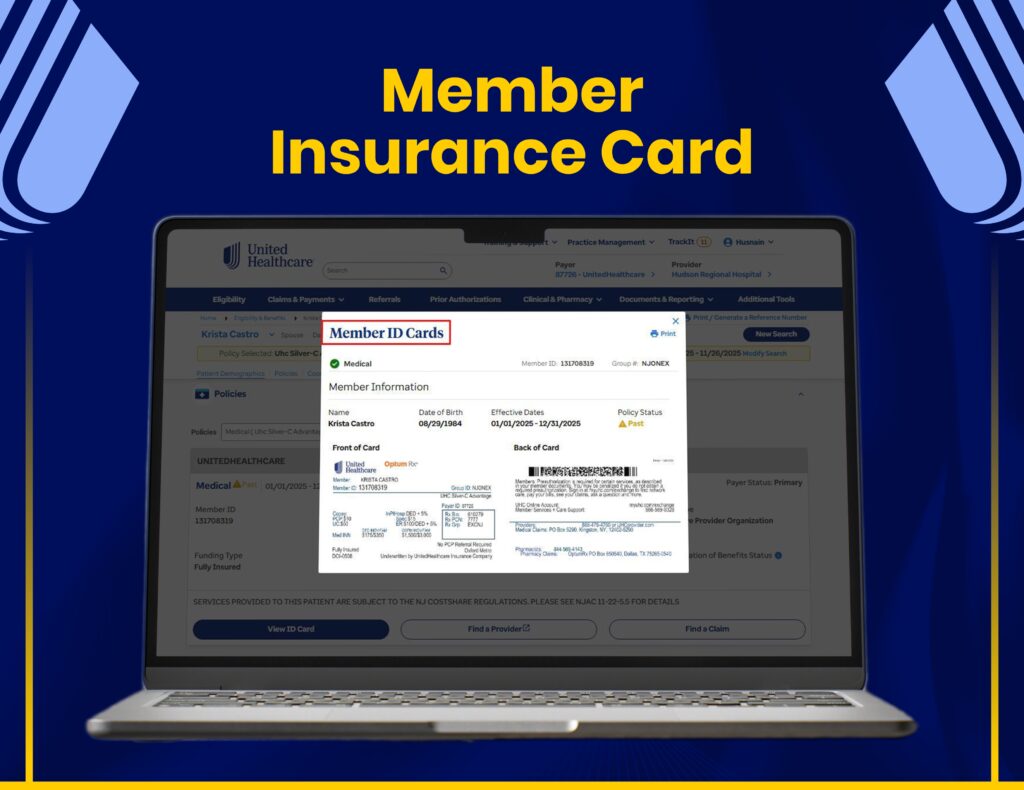
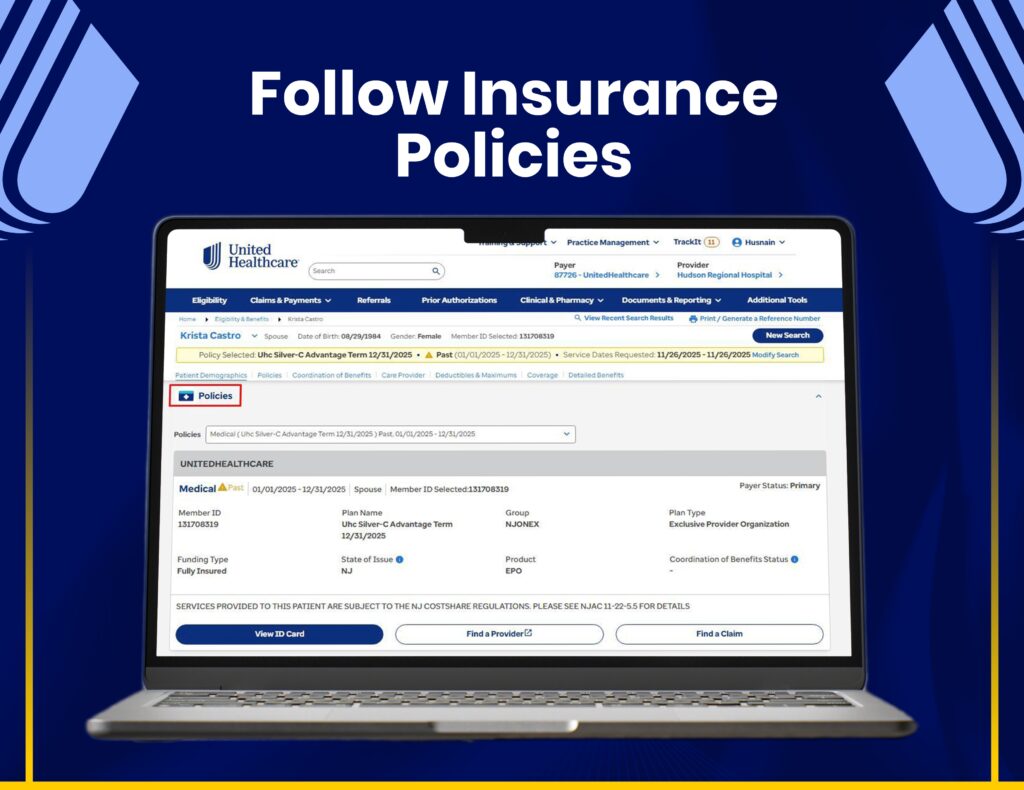
AR Follow-Ups & Payment Recovery
We manage claim tracking, AR follow-ups, and payment recovery through United Healthcare systems to maximize reimbursements.
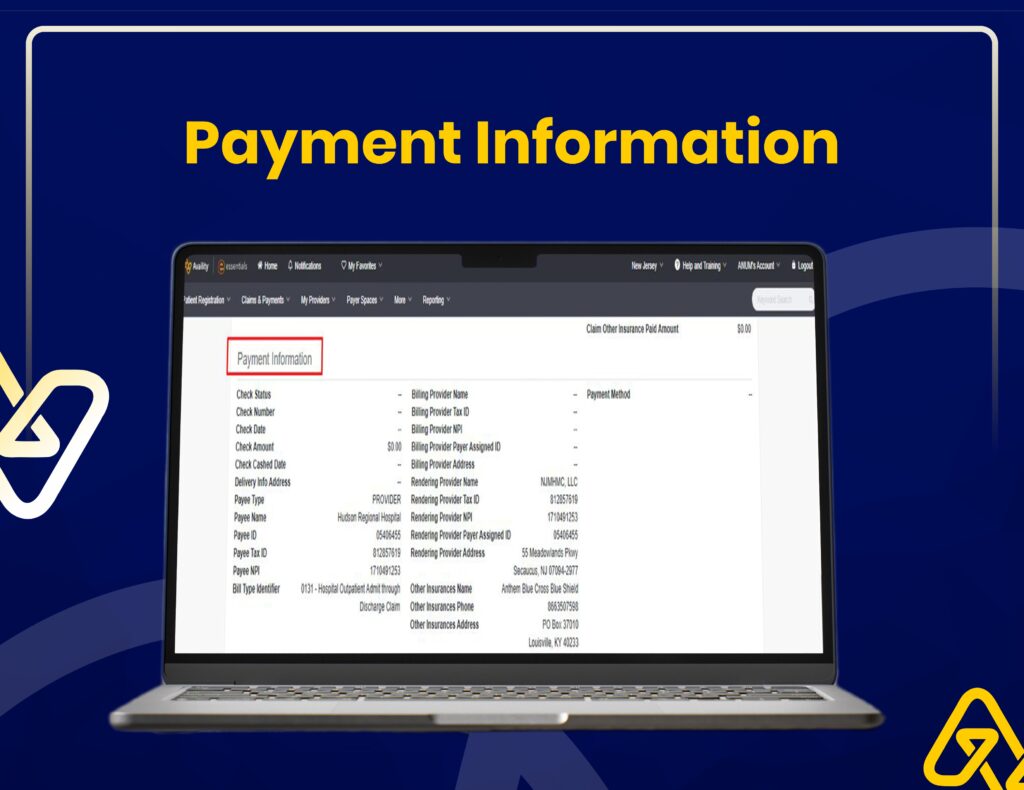
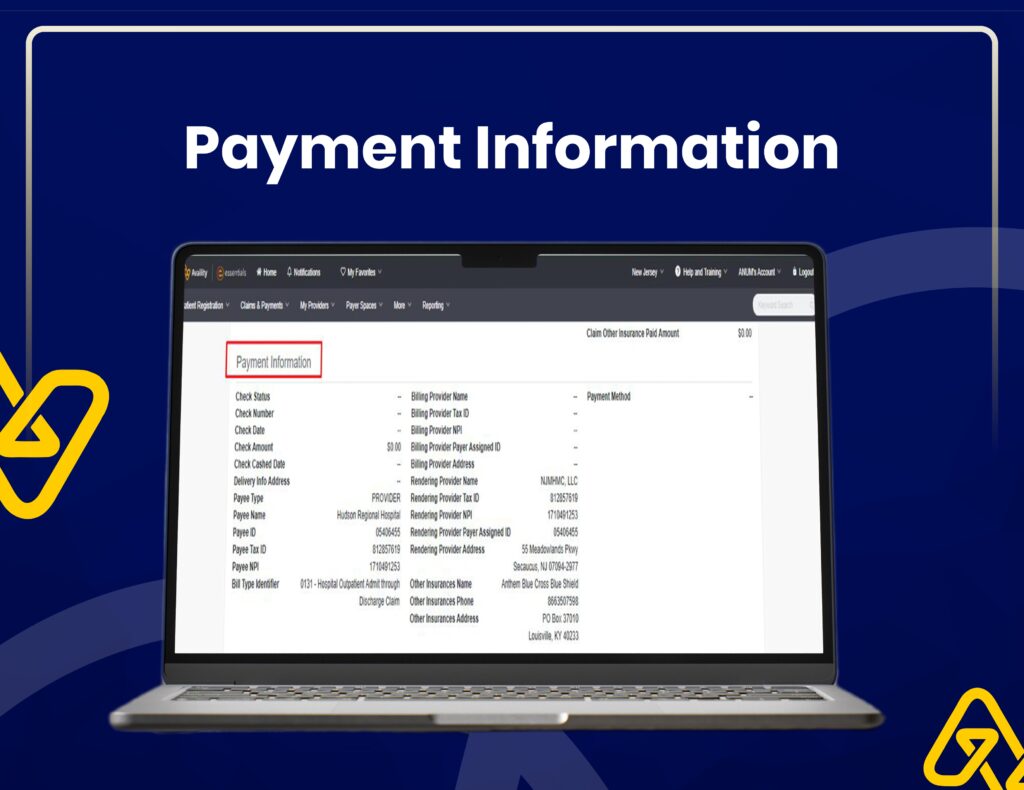
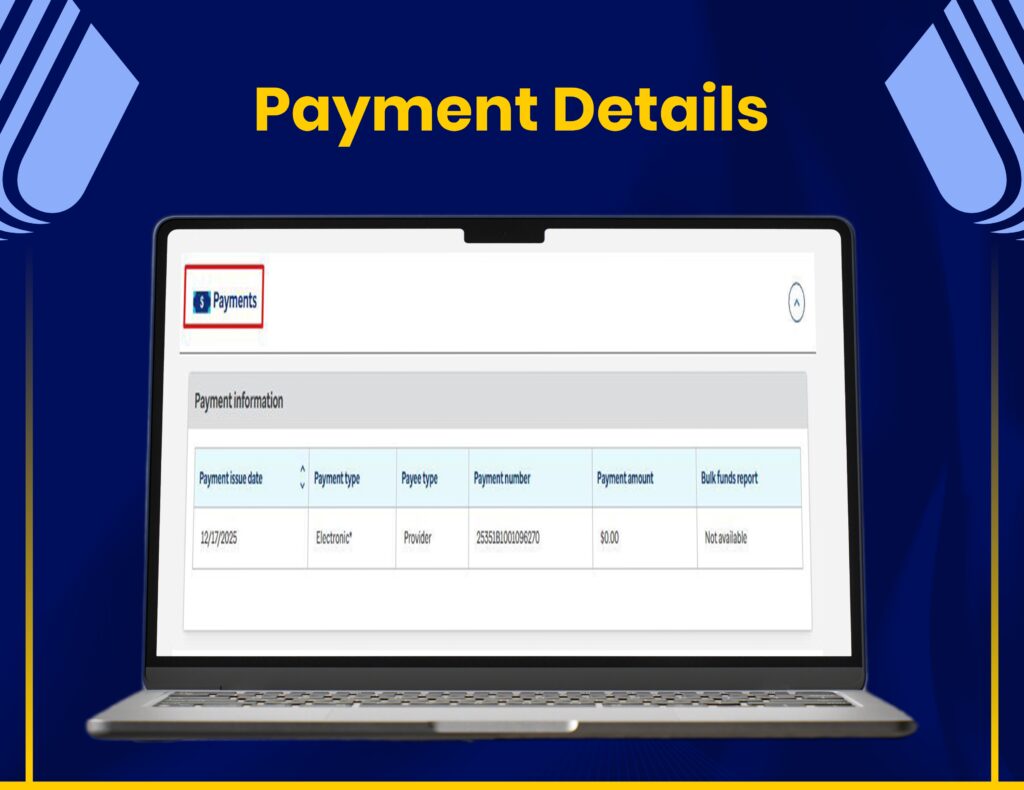
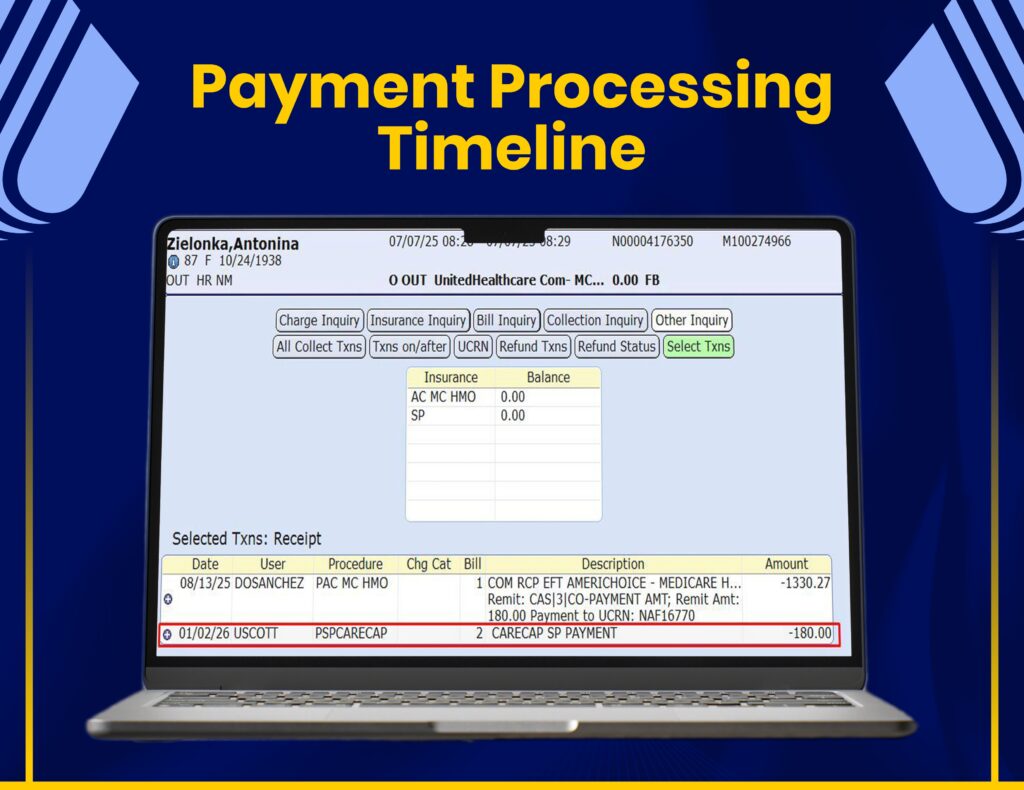
Payment Posting & Reconciliation
Our workflow includes accurate payment posting, adjustments, and reconciliation to ensure smooth financial operations.